Original paper: Soft Matter Science and the COVID-19 Pandemic (arXiv here)
Quintessential soft matter problems, such as the behavior of droplets in ink-jet printing, involve complex interactions between forces and materials. In today’s article, Prof. Wilson Poon points out that coronaviruses are also quintessential soft matter objects, and highlights a range of areas where soft matter science may help better understand, and combat viral pandemics.
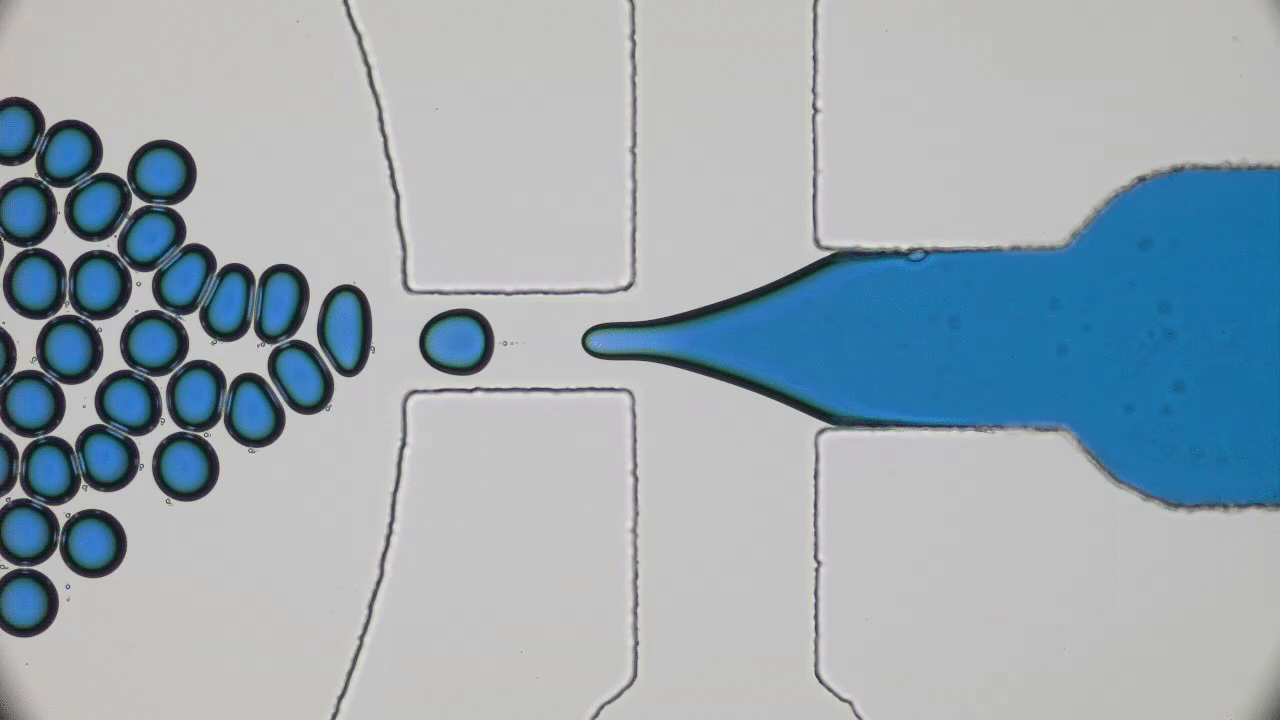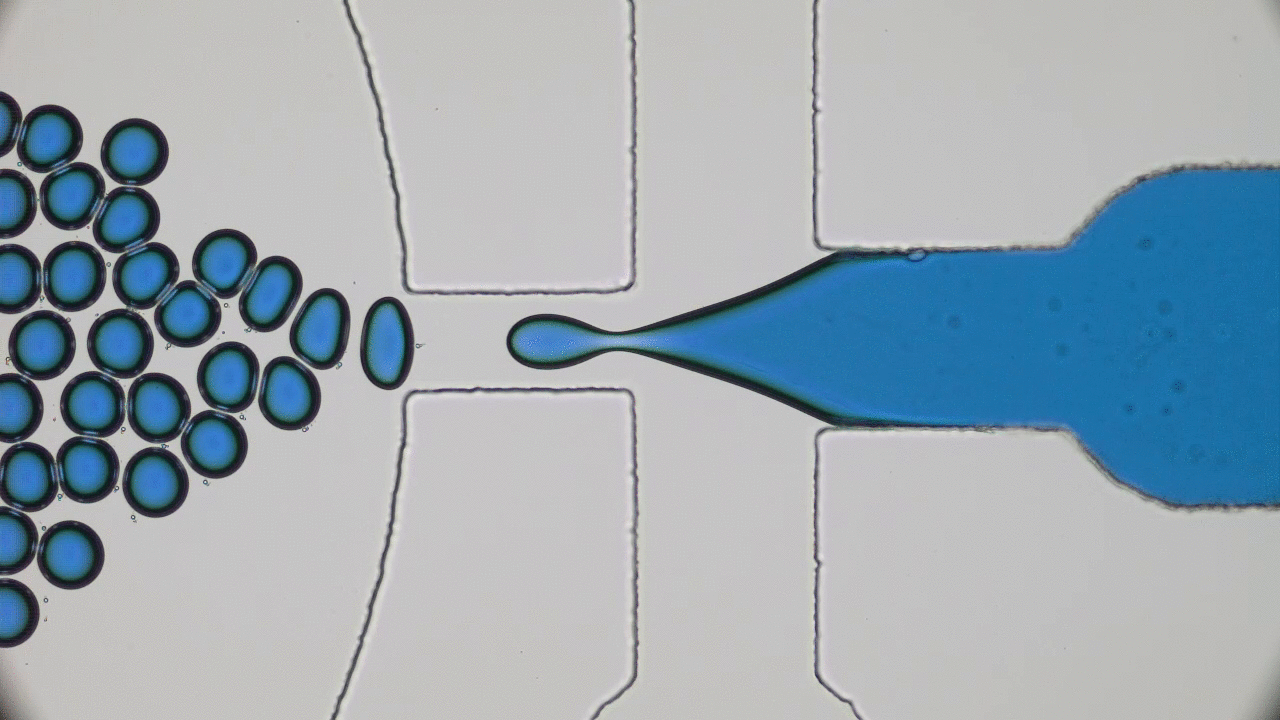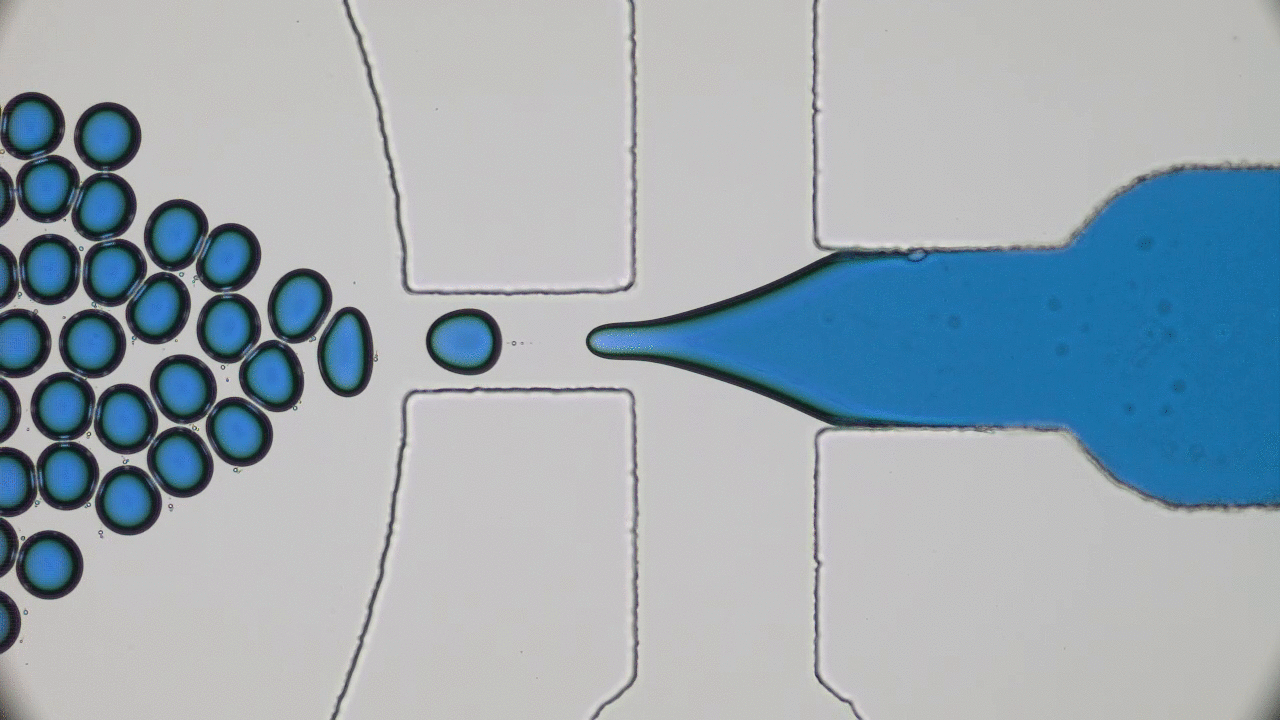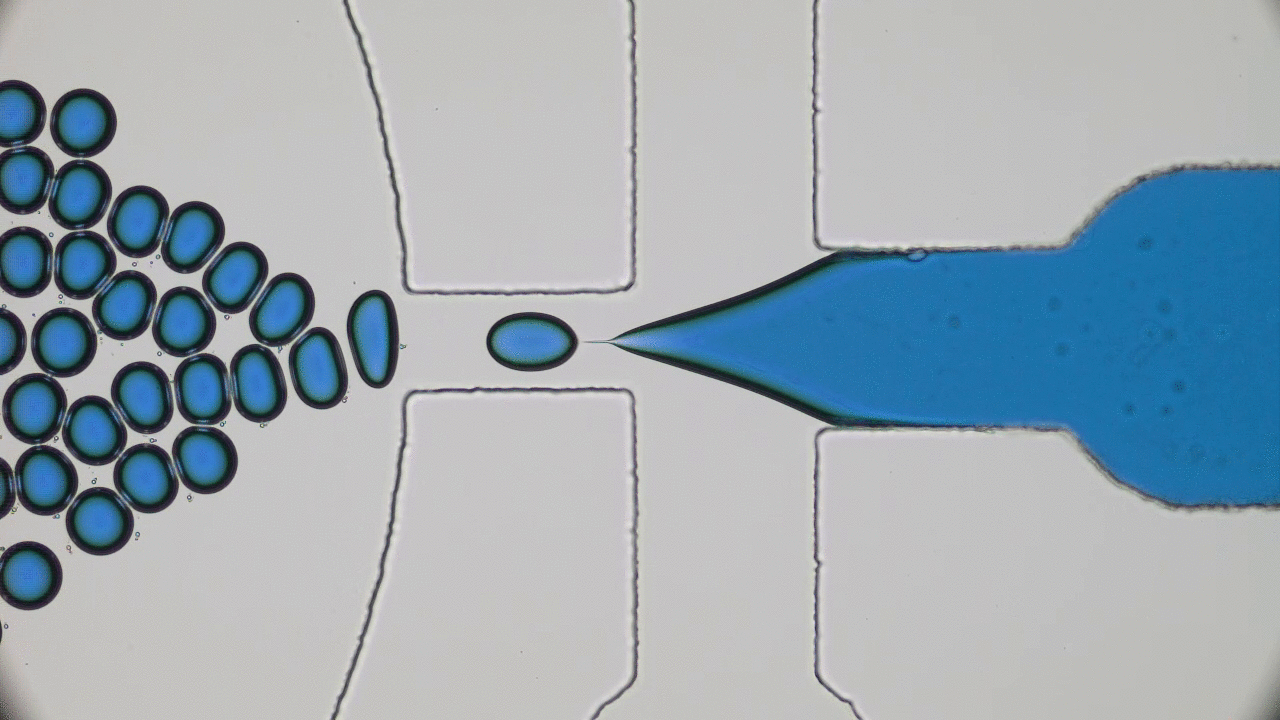
To a physicist, a virus is merely an inert particle that drifts around in water (it is a colloidal particle, in the jargon of soft matter physics, see Figure 1), where a single coronavirus particle is roughly spherical and around one tenth of one thousandth of one millimeter in width (). These inert particles, however, are also covered in tiny specially shaped keys (proteins), and when these keys meet the correctly shaped lock (a receptor at the surface of a cell membrane), they activate. The previously inert particle now instructs the invaded cell’s machinery to make more viruses (imagine a Ford car whose only job is to drive into Rolls Royce factories and rewire the machines to make more Fords). Sickness is then caused by the cells being too busy making viruses to do their jobs, eventual cell death, vast numbers of obstructive virus particles, and the body’s own army of immune response units.
Although less interesting biologically, while in the inert stage the virus has to “survive” a variety of physical conditions, and ideally this is where we want to destroy it, before it has a chance to invade a cell — before the Fords can find the Rolls Royce factories. In this article, we will focus on a number of open questions about coronaviruses prior to invading a host that soft matter could help answer.

Airborne
It is now established that the “dominant route” by which coronaviruses spread is in airborne droplets, through sneezing, coughing and even speaking. In soft matter physics, airborne droplets have been widely studied, both in industry (for example in ink-jet printing) and in academia (for example in finding the scaling laws that govern droplet formation). We may be able to use the lessons we have learned to ask:
- How are these droplets created?
- Does the behaviour of these droplets impact virus survival and transmission?
- Do all droplets contain the same number of active virus particles?
- Can we modify the air to inhibit viral transmission via the behaviour of these droplets?
When sneezes are observed using high-speed photography, as in this video, an image of a turbulent cloud of droplets is revealed. These droplets break apart, collide, stretch and break apart again in a chaotic cascade that could exert considerable destructive shear forces on the viruses, but it is currently unknown whether the turbulence decreases the active virus concentration or if the virus particles influence the droplet break-up events. Solving this unknown may change the way we understand the role of air flows from ventilation systems in inhibiting active viruses.
Despite the lack of information on virus viability in the turbulent sneeze cloud, Poon and colleagues point out that studies suggest that the viral load of virus-carrying droplets is small – around 1 viable virus particle per droplet. However, sneezes typically generate up to 40,000 droplets, whereas a single cough (or talking for 5 minutes) will generate up to 3000. One also needs to know how many viruses a person must absorb before their dose becomes infectious – the minimum infective dose (MID). For the flu, the MID is reported to be around a few thousand, but the equivalent figure is not known for coronaviruses. All of these numbers play a role in infection but collectively point to the importance of limiting the amount of direct droplet transmission, and the importance of ventilation.
Finally, an airborne droplet containing a virus evaporates, at a rate depending on the local humidity, and will eventually completely dry. Interestingly, studies suggest that bacteriophages (viruses that invade bacteria) are more likely to survive in very dry or very humid air, but not in between. The reason for this seems to lie in how dissolved salt destructively interacts with the virus at steady (not slow or fast) evaporation rates. Other saliva components (like the gelation of the mucin proteins that make mucus slimy) also impact evaporation, further complicating the problem of viral transport and survival, but these clues indicate that controlling air humidity could be a viable option for hampering the virus.
On Surfaces
In the previous section, we’ve seen that how droplets behave in the air seems to be important, and this has been well-studied in a variety of commercial and academic contexts. As in ink-jet printing, we should also consider how droplets impact surfaces, as contact from surface to skin to mucus-membrane is another route through which viruses spread.
Here we will summarize the five main questions highlighted by Poon and colleagues in how droplets interact with surfaces, which could be important for understanding viral survival and transmission:
- Splashdown. While ink-jet printed droplets need to avoid bouncing off surfaces, in a pandemic we ideally want the opposite. Polymers are known to give an anti-bounce property to droplets, but do mucins in saliva also have this effect? (see Figure 2 a)
- Coffee rings. Much research has been done on the coffee-ring effect (When Espresso Evaporates), where suspended material is dragged to a droplet’s edges as it dries. Do viruses cluster at the edges in this way, and do these dragging forces impact their viability? This is further complicated by the salts and mucins present in these droplets, which will also accumulate at the edges (see Figure 2 b).
- Material. Surfaces can have complex structures (smooth, ridged, or fibrous) and variable chemistry (metal, glass, or oily skin cells). Interestingly, virus viability tends to follow an exponential decay once on a surface, but the decay rate is higher on some surfaces (e.g. copper) than others (e.g. plastics). A question remains: is this due to a chemical catalytic property, or are some surfaces retaining moisture better than others?
- Capillary Bridges. Watery bridges can form when two wet surfaces come into close contact, but do microscopic bridges form when your skin comes into contact with surfaces, and do they enhance viral transport? Interestingly, bacteriophages are known to better transfer from surface to surface in humid environments, which suggests that such liquid bridges may be important (see Figure 2 c).
- Fluidic Forces. It is well documented that bubbling gas through a solution or filtering it through a bed of glass beads deactivates viruses, but why? Poon argues that there could be significant capillary forces (which are known to deform latex particles in drying paint) pulling on virus particles if they get stuck at the interface between air and water, which will likely happen often in a vigorously bubbled or filtered solution. The behaviour of colloidal particles at interfaces is a rich area of ongoing study, so answers here are anticipated soon.

Final Note
The possibility of a global viral pandemic had been predicted by scientists for decades, and yet was not prevented, and the current one is seemingly unlikely to fully disappear in the near future. While the world’s hopes currently rest with developing and deploying effective vaccines, we should in parallel use every single weapon at our disposal to understand and treat the causes and symptoms of viral pandemics. The lessons we learn may also allow us to improve on some of the problems that the current measures are creating, such as the unfortunate and unsustainable use of single-use plastics in disposable protective gear that contribute to the “plastic pandemic”. Soft matter science may not be central to solving the problem of COVID-19, but is important, and could have a significant role to play in preventing the next global pandemic.