Direct insulin injection is considered a traditional treatment for the type II diabetes. Aside from its painstaking process, this treatment imperfectly regulates the dynamics of insulin release. In this post you will read about designing an artificial cell that can manage to release insulin on-demand when needed.
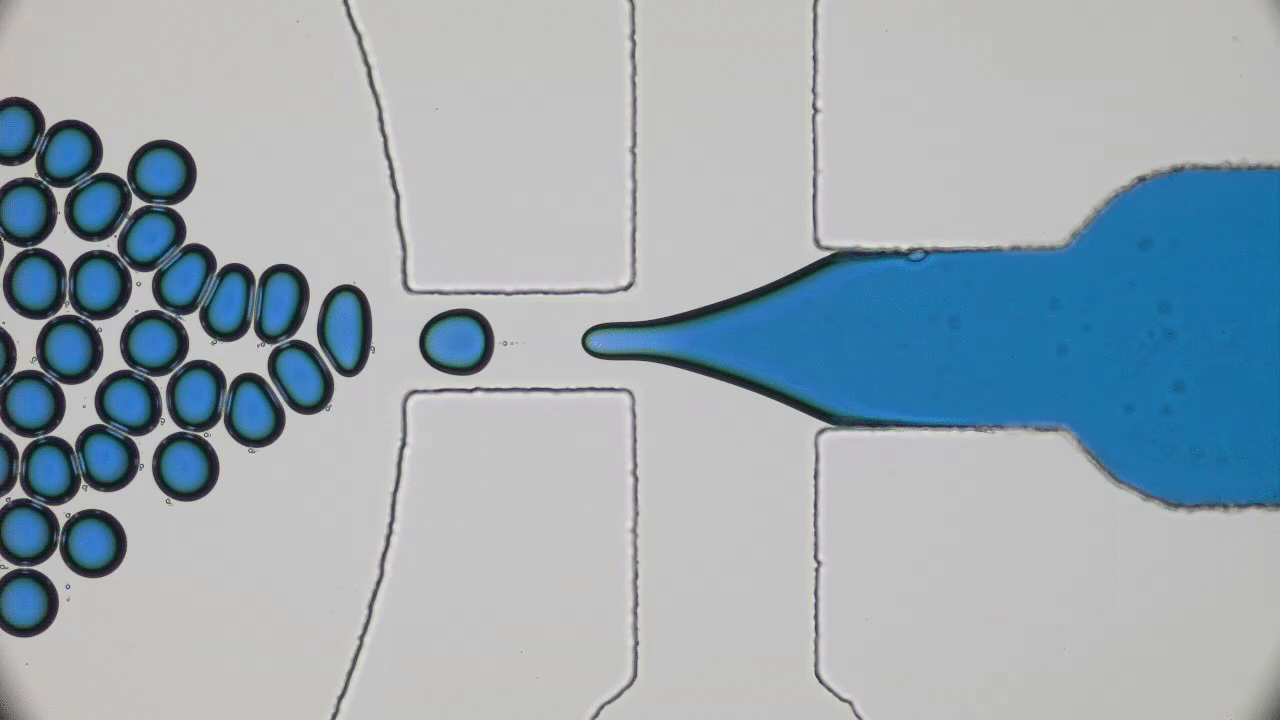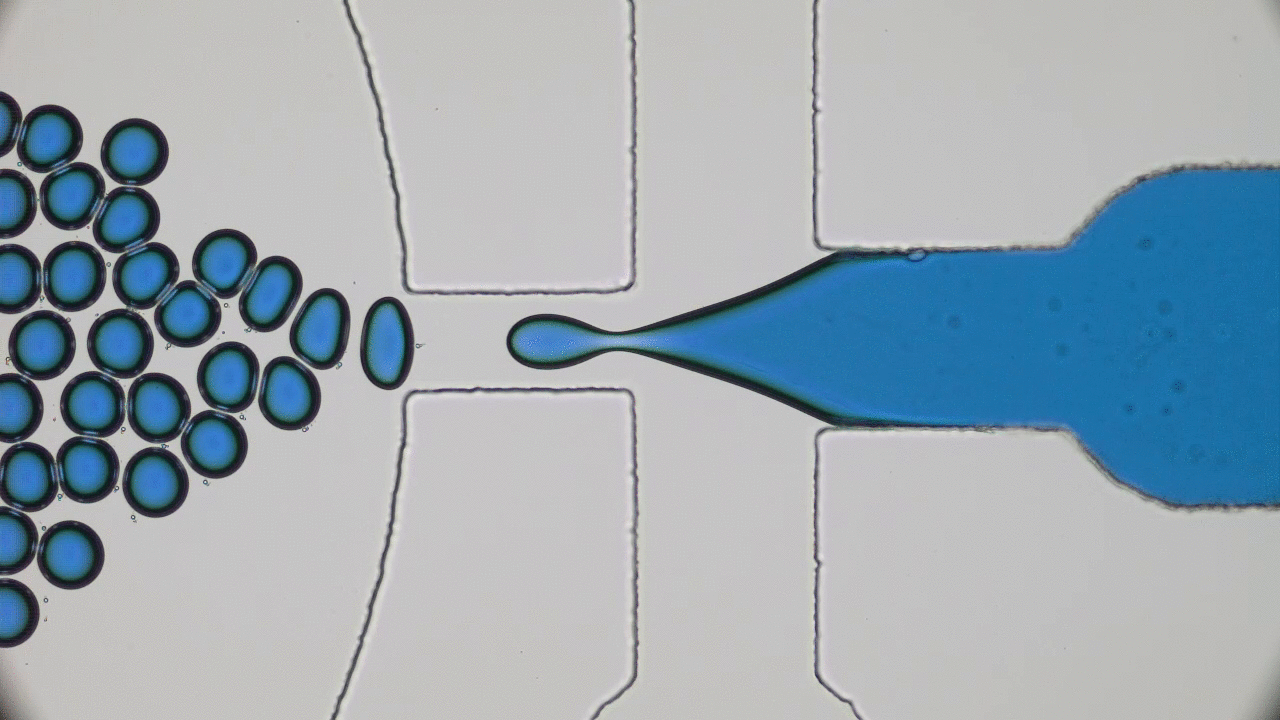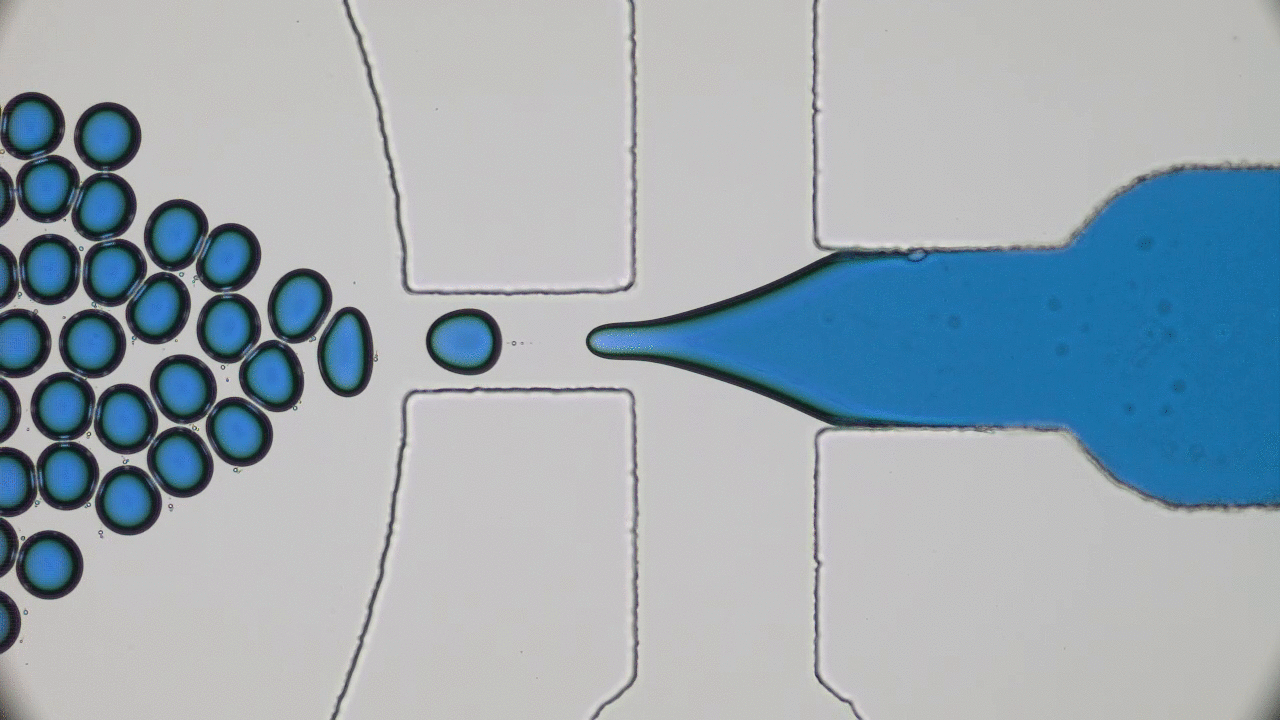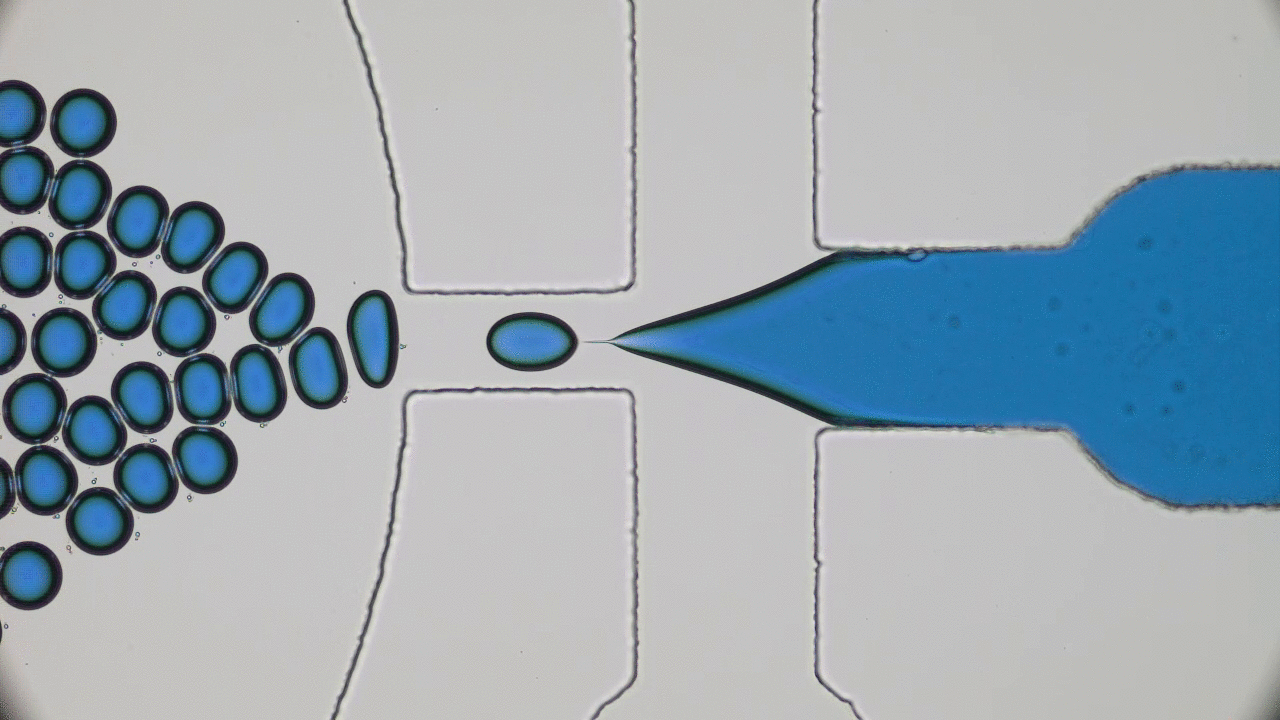
Dripping, Buckling and Collapsing of a Droplet
Cell membrane is evolved to be flexible rather than rigid. This fluid 2D sheet plays a key role in cells’s survival, be it tailoring the nutrition trafficking or rendering a mechanical toughness. In recent decades, however, artificial membranes have been developed with enhanced mechanical properties. Of such systems are particle-stabilized emulsions and in this post we will look into characterizing mechanical strength of such emulsion.
Brick-by-brick to Build Tiny Capsules
In past two decades, several approaches have been developed and optimized to encapsulate a wide variety of materials, from food to cosmetics and the more demanding realm of therapeutic reagents. Inspired by biological cells, the first attempts were to use either natural or synthetic lipid molecules to form encapsulation vessels, i.e., liposomes. Then, with the increasing awareness of controlled release of cargo, especially for therapeutic purposes, advanced materials such as polymers were developed to form carrying vessels. Despite the enormous progress in encapsulation technologies, however, these methods can be limited in their applicability regarding encapsulation efficacy, permeability, mechanical strength, and for biological applications, compatibility.
When Bending Comes at A Cost: Vesicle Formation and Size Distribution
Cells use tiny capsules called vesicles to uptake nutrients, to dump waste, and to communicate. They astonishingly alter the mechanics and size of these capsules that are made of very thin layers with an incredible efficacy and speed. But what are the key parameters that govern the formation of these vesicles?